
Blog, Heel Pain, Shockwave, Sports Care
Blog, Uncategorized
Morten’s neuroma Vs plantar plate
If you’ve ever suffered from pain in the ball of your foot you’ll know only too well how annoying and debilitating it can be. However, addressing the cause of the pain starts with the right diagnosis.
Two widespread causes of forefoot pain are Morten’s neuroma and plantar plate trauma. While plantar plate tears are less well known and identified, they are clinically prolific.
Morten’s neuroma
A Morten’s neuroma is a nerve injury. The joints around the metatarsal bones rub together causing irritation and swelling, which encroaches on the nerves. The nerves can become damaged and thickened resulting in the shooting, stabbing pain and burning sensation linked with a Morten’s neuroma.
The nerves in the intermetatarsal spaces (between the 2nd-3rd and 3rd-4th toes) are most commonly affected leading to pain in the ball of the foot.
Symptoms of Morten’s neuroma
- A sharp, shooting pain in the ball of the foot (usually between third and fourth toe)
- A burning pain in the ball of the foot that may spread or shoot down towards the toes
- Toes may feel numb or tingle
- Pain is intensified when wearing tight shoes or high heels

Podiatrist and founder of A Step Ahead Foot + Ankle Care Dr Brenden Brown explains, “Wearing high heels or tight fashion shoes compresses the nerve and creates that electric, shooting pain.
“People with foot deformities, such as hammertoes, bunions, flat feet or high arches, are at higher risk of a Morten’s neuroma because these defects generally cause the foot to widen, making it more difficult to find shoes that aren’t tight.”
Treatment for a Morten’s neuroma
Treatment will depend on the severity of symptoms but first-line treatment options include:
- Appropriate footwear—avoid shoes that are narrow in the forefoot or tight in general
- Soft tissue rehabilitation — Soft tissue massage to the Morten’s region can provide some relief from the associated pain
- Soft cushioned orthotics with a metatarsal dome may help reduce pressure on the nerve
- Injections to reduce inflammation, such as cortisone or Prolotherapy
- Surgical opinion is required if conservative measures are unsuccessful
Plantar plate tear
This is the very start of clawed or hammer toes! A plantar plate injury involves the ligament and cartilage attached to the base of and between our toe bones (phalanges). Injury can involve tears, ruptures or distensions. Conservative treatment for this condition is highly effective.
Symptoms of plantar plate tear
- Dull ache or sharp pain under the ball of the foot
- A “V” sign where the toes separate and form a V shape
- Toe lifts upwards (commonly the 2nd or 3rd toe) and may become swollen
- In acute cases the toe becomes thickened or enlarged. Often described as “sausage like”
- Feeling that you have a small stone in your shoe when walking
- The feeling that there’s insufficient cushioning between the toe bones and the ground
- Small amount of callous develops under the metatarsal heads
- Surgical opinion is required if conservative measures are unsuccessful
Treatment for plantar plate tear
- Conservative treatment for this condition is highly effective if caught within the first 6 – 12 months
- Wearing firm, stiff-soled shoe can help alleviate pressure on the joint and reduce the pain
- Cushioned orthotics with a metatarsal dome (often recommended by orthopaedic surgeons)
- Soft tissue rehabilitation, deep connective tissue therapies to the joint capsules and the spaces around this area.
- Deep connective tissue therapies to the extensor and flexor tendons and muscles of the foot
- Serial strapping or taping to prevent the toes popping up or hold them in alignment
Dr Brenden says, “For years Morten’s neuroma has widely been the most common diagnosis for forefoot pain. Yet I find that in many cases, where there is a dull ache type of pain in the ball of the foot, the cause is a plantar plate tear rather than Morten’s neuroma.”
Radiology
Morten’s neuroma and plantar plate trauma are difficult to distinguish between on diagnostic ultrasound.
“When viewed in ultrasound the two conditions without further discovery and without an experienced radiologist can appear the same. The two conditions will often return a hypoechoic mass finding, hence the need for more detailed clinical symptoms and signs accompanying the request.
“Given that the difference in symptomatology between the two is often the key, clinical symptomatology should be included in the radiological request,” advises Dr Brenden.
Related articles
4 hacks to staying injury free this winter sports season
5 hacks to keep ingrown toenails at bay
Your guide to sock solid ankle stability
About us
A Step Ahead Foot + Ankle Care is one of Sydney’s leading foot and ankle clinics. Principal podiatrist and founder of A Step Ahead Dr Brenden Brown (AKA Dr Foot) has been taking care of people’s feet for more than 20 years.
With a background in sports medicine and having served as a former president of the Australasian Podiatry Council, Brenden is a wealth of information when it comes to foot and ankle care.

Blog, Growing pains, Kids Feet

Growing Pains- More than just pain from growing – A case study
Sam is 10-years-old. He’s a great kid who loves being active, but there’s a problem and it’s getting worse. Sam plays football in winter and, in summer, he’s a cricket fanatic. Apart from these regular sports he’s running about at school and is, yes your average Aussie kid!
Sam’s mum and dad brought him into A Step Ahead Foot + Ankle Care because, despite being a very happy and active kid, Sam is waking up a couple of nights a week with pain in his lower legs. When he wakes he wants his mum to rub his legs because they ache and are sore. Sam’s mum Beth has used heat packs and paracetamol which does take the pain away after a while but, as Beth says, “They aren’t fixing the cause”.
A key factor is that fact Sam’s parents recognised that the pain sometimes came on in the night after Sam had quite active days, like sports days or family activities with lots of walking.
Visiting the GP, Physio and Dr Google
Sam’s parents took their son to a GP who sent them to see a Physiotherapist. While the physio was nice and showed Sam some stretching and did a couple of massages, these again helped at the time but didn’t stop the problem from coming back. After chatting to the GP their opinion was that this was “Just growing pains”—something Sam would have to get used to, and that he would simply “Grow out of it”. Frustrated with a fantastic but upset little boy, Sam’s parents felt they needed another opinion.
Sam’s mum Beth jumped onto Dr Google and found herself even more confused. Some parents were recommending vitamin supplements, others recommended oils and others suggested all kinds of home remedies. She then found herself on Facebook asking other parents for help. This is where a friend of Beth’s recommended our practitioners at A Step Ahead Foot and Ankle Care.
Finally some answers
When our practitioners assessed Sam it became pretty clear there was more than just some kind of phantom pain going on. We undertook a detailed walk and run assessment, along with some measurements and testing on Sam’s muscles. Nothing was invasive and everything we do is done in a fun, friendly and non-confronting environment. After a short while we established that Sam’s feet were rolling in a lot and his arches where a little flat. In essence Sam had pretty poor foot posture. What this meant is that the muscles in Sam’s lower legs were over working to try and give his poor foot posture support.
This meant that a big day on his feet, like a family outing, a busy day at school or doing sports caused his muscles to work even harder. This led to them getting sore, not necessarily at the time of the injury, mostly at night several hours after the muscles had rested.
Helping fight “growing pains”
To help Sam we gave him a custom-made pair of orthotic insoles. These are made from a soft material so are very comfortable to wear but provided support for the rolling of his ankle. We took a 3D scan of Sam’s foot and video recorded his walking patterns using our specialised assessment software. The orthotics are then designed using our computer-aided design software. Next step is to make the orthotics, which is done in our on-site Orthotic laboratory by our technicians and overseen by our podiatrist.
After fitting his new orthotics into a new pair of runners that we recommended, Sam headed on his way feeling comfortable to return in a couple of weeks. We prescribed some stretching to work with his orthoses and suggested that we may need to follow this up with a specialised massage to relax his muscles as his orthoses took over and began doing their job.
Pain free!
A couple of weeks later a very relieved set of parents and Sam returned to our clinic. In a little over two weeks the orthoses had started to do their thing. Sam had only had pain in his legs once since starting to wear his orthoses and this was after a very big day, his school athletics carnival! After only a couple of weeks we expected this to decrease so we asked them to return in another month at which time they reported Sam to be pain free!! Sam’s parents also reported that he was much more comfortable at sport as well. They were overjoyed; they had their happy, healthy little boy back!
Growing pains ARE TREATABLE in most cases. While many well-meaning health practitioners may say you have to wait and outgrow growing pains, there are alternatives. Our practitioners have had the pleasure of helping many kids with this same problem. It’s what we love to do! Helping kids become pain free, happy, healthy and active is a privilege. If you would like to help your little one to become pain free, please give our helpful reception team a call on +61 9673 2987 or 4732 2007. You can also see find us on our Facebook page https://www.facebook.com/podiatristsydney

Blog, Kids Feet, Sports Care

Blog, Heel Pain, Shockwave
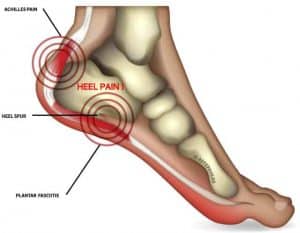
Top 6 reason your heel pain isn’t getting better – UPDATED
You CAN beat Heel Pain
Heel pain can be debilitating! The pain often stops people in their tracks first thing in the morning! Walk a few steps and it may be relieved. Others as the day progresses, the pain becomes worse. Finding help can be frustrating and confusing as you can often see multiple practitioners and receive multiple answers with little relief.
We first wrote this article in 2014. 3 years later, after helping literally 1000’s more patients with heel pain. After HOURS more of research and implementing significant changes in the way medicine has begun to understand Heel Pain, it became time to updated this very popular article!
With the experience of literally helping 1000’s of heel pain patients, between 10 and 20 a day! We have put together the following list of the Top 6 reasons we have noted patients have not got better.
We hope this helps you on the way to beating your heel pain.
1.You decide to go it alone and NOT get professional advice.
Of all the people we see, a large proportion of them have never had any care or professional advice. Quotes like “I just thought it would go away” or “A friend told me what they did to get rid of the pain and I just tried that”. Most times it doesn’t! You will increase your chance of beating heel pain, significantly by getting a professional opinion. Professional advice and treatment costs money. Yes some people find this expensive however others find it invaluable. It depends on how much you really want to get rid of your very sore heels?
2.You wear thongs (flip flops) because your feet are sore
Wearing thongs, Croc type shoes or even bare feet for many people make their feet feel better initially but all our experience tells us you are doing more damage. The pain you feel days later not necessarily at the time. You are welcome to argue this point as much as you like, while you continue to hobble…………
3.You get advice and then choose which bits you use.
Great work on getting advice now it’s time to take it ……yes ALL of it. When a care plan is developed for you, if you choose only the bits you like to hear and the easy bits, you will end up failing to get better. Your Podiatrist should work with you as a patient to establish the best way to relieve you of your pain. They should speak to you about what shoes are best for you. What treatment will get you better quickest, including strength exercises, therapy to relax the soft tissue and possibly orthotics. Now choosing NOT to do some of the suggested treatment universally ends up with patients not getting better. Our Podiatrists do all that and more, does yours?
4.You bought hard rigid orthotics from a Podiatrist.
Our experience tells us that rigid hard orthoses on most occasions irritate the heel and the arch region adding to your discomfort. We have over the years collected many pairs of rigid orthotic from patients who give them to us in frustration after finding they have hindered rather than help. Secondly if this is the only therapy you were given, with the exception of a couple of possible stretches then we would suggest to you that there is more to getting rid of your pain than this – ask the question “So how is this rehabilitating my damaged soft tissue?”
5.You stop ALL activity.
As our understanding has changed over the years we now appreciate the following – “TENDONS HATE CHANGE”. Stopping all activity if you are currently active is a sure-fire way to ensure that when you return to your activity you will also see the return of your heel pain!
You SHOULD make modification to activity, However a complete stop will mean you either
A. Need to rebuild your activity over quite an extended time.
or
B. Your heel pain is likely to return!
For the moment STOP Jumping of and onto things. For example, on + off a truck, box jumps at exercise class, skipping or other high intensity impacting the heel and forefoot until we have you back to comfortable. We will then slowly load you back up to these activities.
6.You choose a practitioner who does not understand heel pain.
So your GP says they will fix your heel pain? Your Physio who is treating your shoulder says the same and the Podiatrist you see, who works one day a week at your local GP clinic and cuts your toe nails, says they will fix it no problem. Who do you choose?
Your heel pain is not simple its complex and for you it’s really sore! Choose someone who see’s and treats heel pain regularly. Choose someone who is passionate about making sure that they help you on the way to getting you better. All the people above are probably very good at what they do, but they most likely won’t end up helping you beat your pain!
Did you know there are about 10 different condition’s that could be causing your pain? When our practitioners are asked by GP’s Physio’s + Podiatrists on Heel pain it is often a surprised to the how complex this condition is! Our Doctors all sports podiatrists see this condition multiple times a day. When you see something that often you are more familiar with it + know how to get on top of it. Ask the person you see how many Heel pain patients they help a day.

How can we help
At A Step Ahead foot + Ankle care we see approximately 8 to 12 heel pain patients a day. We have patients that travel literally hundreds of kilometres to seek our help – Which is really lovely! Our clinics are set up quite specifically to treat patients with heel pain. We have invested hundreds of thousands of dollars into equipment and the latest technology to help us, help you- beat heel pain.
Our Principal Podiatrist Brenden Brown is recognized as an expert in Podiatry. A past President of the Australasian Podiatry council he is considered a Medical Expert in the area of Foot health, appearing regularly on television shows like the Today Show and Magazines like Men’s Health. He has appeared for some time as the Medical expert for lower limb conditions on ABC radio’s “the Waiting Room”
It would be a pleasure to help you beat your heel pain.
We are located in Penrith and St Marys in Sydney’s Western suburbs.
You can contact us on 47322007 or 96732987 we hope you will.



 Frustrated with this she saw her GP who suggested she try putting some ice on the area. Again, she went home determined to get better but with little result, YUP the ice made it immediately feel better, but straight after on the next walk it came back.
Frustrated with this she saw her GP who suggested she try putting some ice on the area. Again, she went home determined to get better but with little result, YUP the ice made it immediately feel better, but straight after on the next walk it came back. You don’t have to put up with Foot pain! There are answers other than waiting for it to go away and pills! At A Step Ahead we see dozens of people like you with foot and lower limb pain all day and we love it! We love getting people better so they can kick their health goals whether its running 5 km or 50 km’s or if it’s professional sport or simply ridding yourself from foot pain so you can play in the park with the kids!
You don’t have to put up with Foot pain! There are answers other than waiting for it to go away and pills! At A Step Ahead we see dozens of people like you with foot and lower limb pain all day and we love it! We love getting people better so they can kick their health goals whether its running 5 km or 50 km’s or if it’s professional sport or simply ridding yourself from foot pain so you can play in the park with the kids!



















 Dr Brenden’s White paper report on the “6 Reasons You Won’t Beat Heal Pain” outlines what’s stopping you from beating this and tips on how to stop it in its tracks!
Dr Brenden’s White paper report on the “6 Reasons You Won’t Beat Heal Pain” outlines what’s stopping you from beating this and tips on how to stop it in its tracks!